Question: My doctor told me that my husband’s sperm and my egg quality were poor. Does it mean that I have no chance of getting pregnant with IVF?
Dr Helena’s Answer:
To achieve a successful pregnancy, may it be naturally or through assisted reproduction techniques, requires some basic pre-requisite factors:
(1) good quality and quantity of eggs and sperms to make good quality embryos
(2) a conducive uterus environment for implantation
In some cases whereby the husband’s sperms were poor in quantity & quality, whereby natural conception is virtually impossible, a Intracytoplasmic sperm injection (ICSI) technique to fertilize eggs during an IVF cycle overcomes certain degree of difficulty to create an embryo. However, if the sperms are extremely poor in quality, there are good scientific evidence to suggest that Fertilization and cleavage rates, quality of embryos as well as blastocyst development rates were significantly reduced, as semen quality decreased.
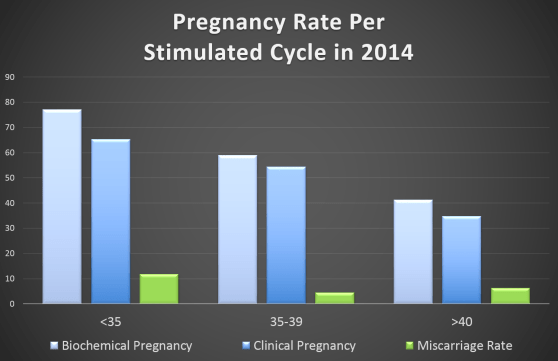
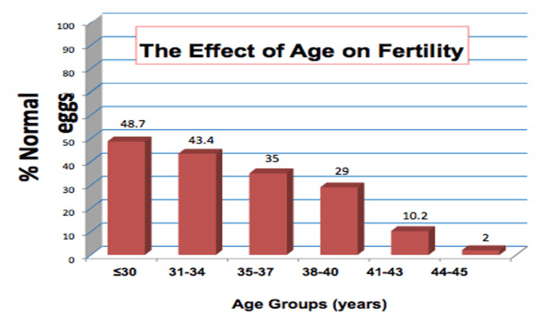
An IVF cycle can also be unsuccessful if egg quality is poor even with good numbers of eggs (and embryos). Egg quality reflects about 95% of the final quality of an embryo. Poor egg quality, therefore, always leads to poor embryo quality. The quality of sperm, while not unimportant, is nowhere near as important as egg quality.
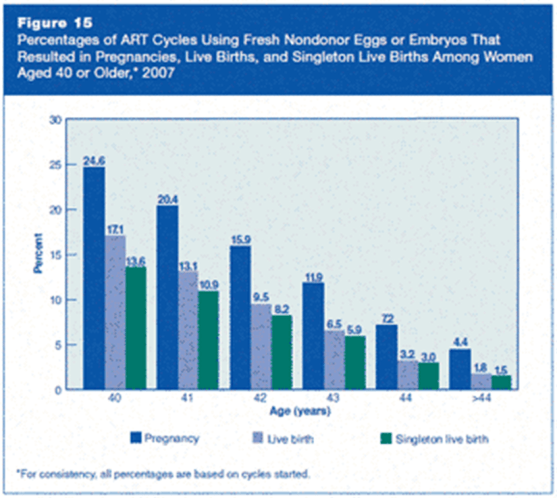
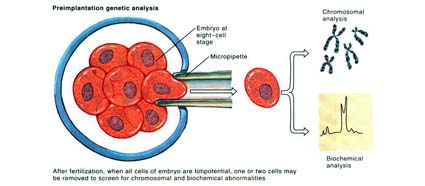
Embryos from low-quality eggs often fail to develop properly. In an IVF cycle, embryos are observed for 3 to 5 days as they grow, before they are transferred into the uterus. On the third day, good-quality embryos should reach 6- to 8-cell stage, and have a more or less regular shape. Embryos that don’t reach this stage within the first few days of development cannot be used for embryo transfer. In addition, some embryos that do reach this stage may be aneuploid (have chromosomal abnormalities). Aneuploid embryos, if they implant at all, are usually miscarried early in the pregnancy, thus also resulting in “failed” IVF.
Therefore, as many of our patients already know, it is not just the number of eggs that is important. The quality of eggs is also crucial for the success of IVF.
Although some people are born to have poor sperms or eggs, majority of poor sperms and eggs can be improved by various means. Change of lifestyles such as stop smoking, stop alcohol intake, exercise moderately, weight reductions, good quality sleep, good nutrition by taking balanced diet, taking food rich in anti-oxidants, acupuncture and etc are some of the strategies one can employ to improve sperms and eggs quality.

Numerous studies had shown that with these improvements in lifestyle, the success rates of IVF in these group of patients improve remarkably.
Therefore, if your doctor had commented that your sperms and eggs are not good in quality, it maybe a good idea to look into your lifestyle and food intake to improve your chances of pregnancy.








 When it comes to family planning, women bear a disproportionate amount of the responsibility. There are very few male methods for family planning that are both practical and effective. Consultant obstetrician and gynaecologist Dr Helena Lim explores what’s on the horizon for safer and better family planning methods.
When it comes to family planning, women bear a disproportionate amount of the responsibility. There are very few male methods for family planning that are both practical and effective. Consultant obstetrician and gynaecologist Dr Helena Lim explores what’s on the horizon for safer and better family planning methods.