Category Archives: ICSI
IVF after the age of 40 & Gender selections
Question: I am current 40 years-old and would like to know what is my chance of getting pregnant with IVF. Can I choose the gender of my baby when I go through an IVF
Dr Helena’s Answer:
One of the biggest single determining factor for IVF success is the woman’s age. Before the age of 35, the IVF success rate is around 60-80%. After the age of 35, the success rate drops to 40-60%. The success rates of IVF drop drastically after the age of 40 to about 20-30% and then 1-2% after 45.
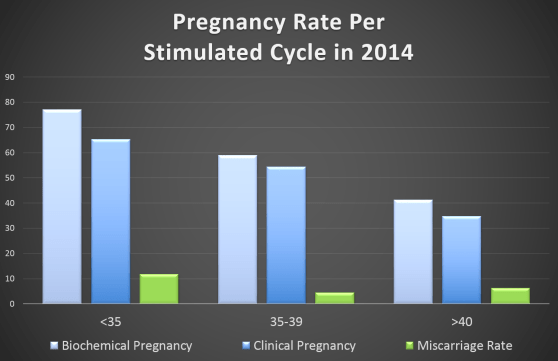
The reason for this is because as women aged, the number of follicles produce each menstrual cycle drop drastically. The quality of eggs also deteriorate as we age. As we aged, the division of chromosomes in our ovaries can become more imperfect, resulting production of eggs with faulty sets of chromosomes, leading to increase number of abnormal eggs and henceforth abnormal embryos.Therefore, women over the age of 40 has a lower rate of pregnancy with each individual IVF cycle, compare to their younger counterparts
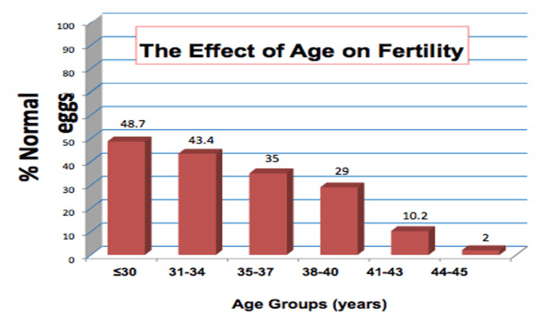
This is a macroscopic view of the general population of women after the age of 40. However, an individual’s success rates is also dependent of her body condition, her ovarian reserves and her uterus receptivity. No two women at the age of 40 is exactly the same. A healthy 40 year-old woman with good ovarian reserves is more likely to produce good number of good quality embryos. Her counterpart who smokes and drinks, eats badly and have poor ovarian reserves is more likely to fail her IVF attempts.
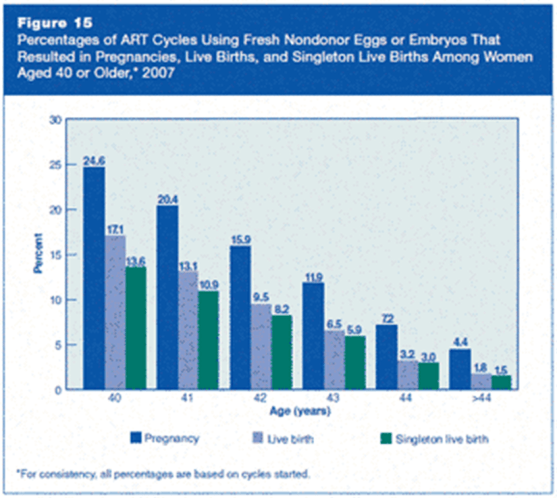
Recently, advances in Pre-implantation Screening (PGS) tests allowed us to biopsy embryos at blastocyst stage to select embryos which is normal in chromosomal make-up before embryo transfer. This test is extremely useful in determining which embryo is more likely to get our patients pregnant. However, like all the tests in this world, it comes with its problems as well. First and foremost, PGS is still expensive, and this test can only be done on embryos created from IVF, which then increase the cost of the IVF cycle. If the embryos tested showed that all the embryos are abnormal, there is no way we can change or treat these embryos and make them chromosomally normal. And therefore, some patients may end up not having any embryos which is suitable for transfer after an IVF with PGS. However, if this is the scenario, the couple can then move on quickly to another cycle of IVF to collect more embryos for PGS, hence, shortening the time required to find the ‘right’ embryo to achieve pregnancy.
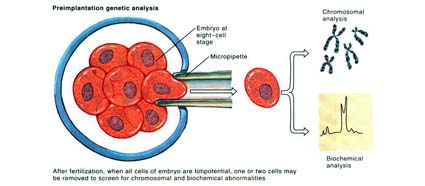
Although this technology is able to reveal the gender of the embryo, one must realize that the use of such technology to perform gender selection in STRICTLY Prohibited in this country and also most countries in this world. It is important to note that IVF and PGS are technologies to help couples to achieve a healthy pregnancy and must not be misuse for ones’ whims and fancies. Science and technology should be use sensibly to maintain and restore nature’s balances and any manipulation as such can potentially tip off the balance and create potential disasters to mankind.
What is the cause of my Failed IVFs?
Question: My husband and I had gone through 3 IVFs without success, does it mean that our chance of pregnancy is very slim? Is it due to my body condition?
Dr Helena’s Answer: To achieve a successful pregnancy through IVF, there are some basic pre-requisite factors:
(1) The age of the couple, especially the female partner
(2) The duration of Subfertility
(3) good quality and quantity of eggs and sperms to make good quality embryos
(4) a conducive uterus environment for implantation
Studies had also shown that there is a increasing cumulative pregnancy rate for women who went through a few cycles of IVF.
However, after going through three IVF without success, one may wonder whether there is light at the end of the tunnel.
Being a fertility doctor, I can understand how frustrating it would be. However, these IVF cycles which did not work out, may contain valuable information about your fertility. As we know, apart from being a treatment in its own right, IVF also serve as a diagnostic tool in its own right, by telling us how you respond to the medications, how your eggs and sperms qualities are, and how your embryos qualities are.
There a a few aspects we may consider to improve on for your next IVF treatment:
The IVF treatment protocol
The clinic
The sperm
The eggs
The uterus
Here are some consideration for you:
(1) The IVF Treatment protocol.
While the IVF treatment protocol is pretty standard, every patient responds differently to the types and dosage of IVF medication. Each cycle teaches us how your body responds to the injections to help your follicles grow. It takes a good IVF doctor to be able to decide on the right dose and right type of medications, to get you to produce an optimal number of high quality eggs. Some young patients with normal ovarian reserve grow well in response to a standard protocol, patients with poor ovarian reserve and those with PCOS need a lot of extra attention and closer monitoring.
However, at the end of the day, some of this is trial and error. A good previous record can help us to learn from each cycle , until we can customize the perfect protocol for you
(2) The IVF clinic/centre.
It is important to note most IVF clinic/ centre are pretty standard, there are variations in terms of their operations and quality controls, and hence their success rates. In Malaysia, there is still no regulatory body that mandates each IVF clinic/ centre to report their success rates. However, it is important to look for credible centres with proper accreditation to ensure the quality of your IVF treatment.
(3) The sperm.
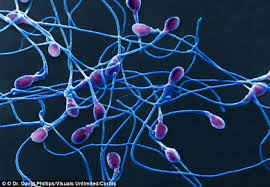
Poor sperm quantity & quality may be associated with failed fertilization of an egg during an IVF but with the advent of ICSI, these problems are easily over-come. However, if the sperms are have high DNA fragmentation, the resulting embryos may still have poor quality. Simple lifestyle changes such as stop smoking & alcohol, weight loose, exercise and consumption of good quality food which are rich in anti-oxidants are some of the key elements in improving sperm quality and IVF outcome
(4) The eggs.
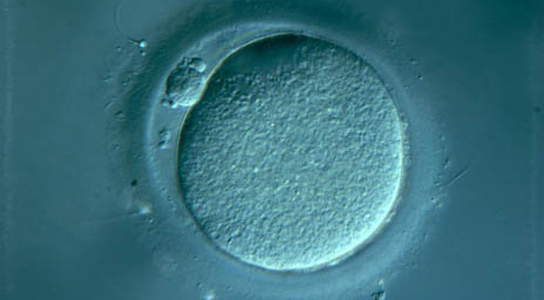
Human egg is a thousand times bigger than the sperm, and that the energy for cell division during embryo cleavage comes from the mitochondria in the egg’s cytoplasm, therefore, egg quality is another important factor for IVF success. Poor egg quality leads to poor embryos and hence failed IVF. The problem is that it’s very hard to make this diagnosis, as there is no blood tests or medical technology to identify poor eggs prior to an IVF cycle. In fact, IVF is a diagnostic tool in it own right, as egg quality can be assess during an IVF. To improve egg quality involves making lifestyle changes, improving diets, and sometimes some alternative medications such as DHEA.
(5) The uterus.

It is probably a very Oriental or ‘Chinese’ believe that failure to get pregnant/ implantation is always the fault of the uterus. It is not unusually to hear the terminology of ‘cold uterus’ being cited for the reason for not getting pregnant. Hence, the idea of surrogacy has become very popular recently because of the disproportionate amount of media attention it attracts, and especially so when cross borders IVF had become extremely popular with the ease of medical access overseas. This had lead to the idea that the best medical solution for them after many failed IVF cycles is surrogacy. After all, the fact that the embryos are not implanting means the uterus must be ” defective” , so doesn’t it make sense to use a fertile woman’s uterus as an incubator for 9 months ? However, the truth is that surrogacy is an expensive and complex treatment option, which is best reserved for women without a uterus. It is also important to stress that Surrogacy is ILLEGAL in Malaysia. Research shows that the reason for failed implantation is much more likely to be genetically abnormal embryos ( because of poor quality sperms or eggs), rather than a uterine problem. However, in about 20-30% of women, failure in implantation maybe due to some small correctable issues in the uterus such as polyps or fibroids. These issues can be dealt with easily without having to resort to surrogacy
Is IVF Painful?
Question: I am a person who is fearful of pain. I gathered that going through IVF will required multiple injections, surgery and other procedures which are painful. Is it true?
Dr Helena’s answer:
IVF sounds daunting to many people. A lot of us have perceptions that it is extremely expensive. Some of us thinks that it would bring us a lot of inconvenience, such as having to go to hospital everyday, lay in bed for a few months, quit our job and etc
One of the greatest fear many had was the perception of pain associated with IVF procedures. The thought of having daily injections made most of us wanting to run away and hide from the doctors. Some people are scared thinking about the egg retrieval procedures. Some are dreading the embryo transfer procedure, thinking that it would bring great pain and discomfort. Some dread the injections which are taken after the procedure, which are the progestogen injections, aimed to support the lining of the uterus whilst the embryos are implanting.
However, with the new development and breakthroughs in the world of reproductive medicine, IVF procedures had become more and more comfortable and easy to management, with minimal disruption to daily life.
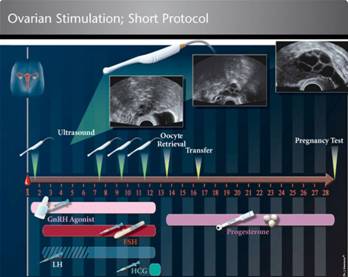
First and foremost, the durations of injections had been shortened significantly with the use of antagonist injections in IVF. This method of doing IVF is called the antagonist cycle or the short protocol. So, instead of having 3 weeks of injections in the agonist cycle or long protocol, the advent of antagonist injections had lead to a shortened period of 10-12 days of injections. This had greatly reduce the discomfort one needs to go through with injections.
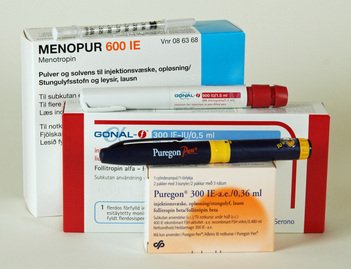
The use of self-administered FSH injection pens with extremely fine needles, had significantly cut down the pain one experienced during injections. This self- administered injections pens are given to patients to take home, and the injections are administered by patients themselves, so patients do not need to come to the clinic or hospital to have their daily injections. The needles used are similar to the ones used in the insulin injection pens, which is extremely fine and almost painless.
There is also another long acting FSH injection which given at the beginning of an IVF cycle and can last for 7 days. After the initial injection, the patient need not take FSH injection for the next 7 days, which significantly cuts down the number of injections required.

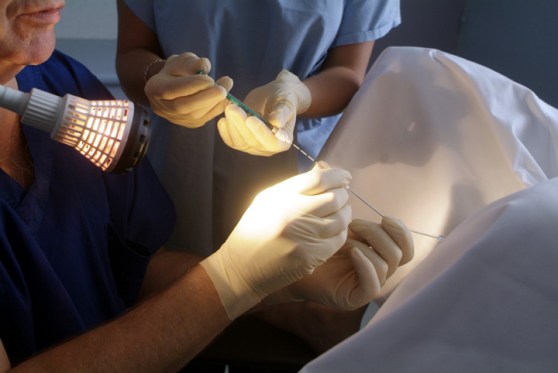
The egg retrieval procedure which usually happened after 10-12 days of injections involved having a light sedation in an operating theatre. In the past, the use of certain sedations such as Valium, Dormicum or pethidine administered by the IVF doctors whilst performing the egg retrieval procedure had appeared to be increasingly unsafe. In many IVF units, a proper IVF operating theatre with a trained Anaesthetist giving sedation during the egg retrieval procedure is becoming a norm and deemed acceptable in terms of safety. One of the advantage of the involvement of an Anaesthetist is that egg retrieval procedure is becoming almost painless, and hence optimizing patient experience in IVF.

Embryo transfer procedure is usually carried out 3-5 days after the egg retrieval. During the procedure, the embryos which were created following fertilization of the retrieved eggs with sperms are replaced into the uterus. This procedure is performed without anaesthesia or sedation, is relatively pain free. The experience is almost the same as having a cervical smear. Therefore, women should not feel fearful about having an embryo transfer.
After the embryo transfer, to support the uterus lining and to ease implantation, a
Progestogen is prescribed. In the past, progestogen is administered by injections. These injections are usually painful and cause local irritations, which is uncomfortable and unacceptable to many. With the advent of effective oral and vaginal suppository preparations, studies had shown that these forms of progestogen are equally effective in delivering progestogen to uterus, injectable progestogen had slowly becoming a thing of the past in many IVF centres. This has also greatly cut down the pain experience in IVF
In conclusion, with rapid modernization in reproductive medicine & technology, IVF had become relatively painless. It is importantly to find out more information on IVF before you embark on this journey.

星洲日报:医识力-人多力量大,孩多好办事
妈妈宝宝杂志-女性不孕症
BFM: STIGMA AND MEDICAL CONDITIONS
What do mental health, HIV, and erectile dysfunction have in common? These are just some well-known medical conditions that are still highly stigmatised. Why are some medical conditions stigmatised and how did some of them manage to break the stigma? Upper GI and Bariatric Surgeon Dr Reynu Rajan shares her experience dealing with bariatric patients in the face of weight-bias and discrimination, while Fertility Specialist Dr Helena Lim shares what it’s like to help patients overcome the taboo of infertility.
http://www.bfm.my/reynu-rajan-helena-lim-medical-conditions-stigma.html
8TV – 不孕与助孕疗程
Astro AEC 女人好健康 Good Health Women TV show – 不育不孕的原因和治疗方法 – – 林韵璇医生 Dr Helena Lim
NTV7 活力加油站/亲子休闲 - 不孕不育,问题何在?- 林韵璇医生 Dr Helena Lim





