Tag Archives: IVF
MELODY FM 十方斌管 – 斌纷一家 (6月9日) 人工受孕夫妇的危险性?
为何还没有好消息?- 妈妈宝宝杂志
勿忘精子检查-风采杂志
Unexplained Subfertility
Like most Fertility Specialist, we faced patients with all kinds of fertility problems everyday. One of the most unique group of patients would be those who are categorised as unexplained subfertility.
It is the most frustrating & awful diagnosis for the patients. These patients are generally well but frustrated. The label of unexplained subfertility is a diagnosis of exclusion, which means that these patients had gone through most of the tests for subfertility and all the tests came back with normal results, but yet they are not able to get pregnant naturally.
In general, up to 10-25% of couples will not find any causes for their subfertility after going through fertility testing. This diagnosis can be frustrating as many of them would wonder: why is it they have not achieved a pregnancy given that all the test results had been normal?
The important thing to note is that even though all the tests are normal, it does not mean that there are no factors that prohibit them from having a baby naturally.
It is important to note that most of the fertility tests are mainly simple fertility tests. These tests do not necessarily assess function.
For example, despite showing both of your Fallopian tubes are patent through a dye test (hysterosalpingography, HSG) or a diagnostic laparoscopy, it does not necessary translate that the Fallopian tubes function are good and it does not necessarily ensure normal transport of eggs and sperm in the Fallopian tubes as there has not been a valid test for this. We know that Fallopian tubes were lined with multiple fine hairs (cilia) within the tubes, and the function of these fine hairs is to transport the eggs and sperms to meet at the most suitable place to encourage fertilisation. The cells in the Fallopian tubes also produce secretions to encourage the process of fertilization. Although the Fallopian tubes were patent, if these functions of the Fallopian tubes were poor, fertilization fails to occur. Unfortunately, there are still no tests for these conditions.
There are also conditions whereby there are poor quality of eggs or poor functionality of the sperms which attributes to this diagnosis. As Fertility Specialists, we can visualized the number of eggs you have and measure the hormones which governs egg productions. However, there is no valid test to check the quality of the eggs until the day one goes through an IVF (in-vitro Fertilization) where the doctors and the embryologists would be able to examine the eggs under microscope. Therefore, apart from being a treatment, IVF can be a diagnostic tool in its own right.
The same principle applies to the functionality of the sperms. During semen analysis, we can see the number, the activity, speed and shapes of the sperms. However, there is no test to check whether the sperms can fertilize eggs until the day we perform an IVF using these sperms. Again, IVF becomes a diagnostic test in this scenario.
If you had been diagnosed with unexplained subfertility, my advice to you would be not to leave it for ‘nature to take its course’. There maybe other underlying conditions whereby the current fertility tests available are unable to address the issues or to diagnosed the condition. It is important to put things into perspective and move on with Fertility Treatment.
Cumulative Pregnancy Rates for IVF
I absolutely LOVE to give my patients the news they wanted to hear. ” Yes, Madam XYZ, your pregnancy test is positive”, and I live on the thrills of having them laugh with tears of delights and relief. However, on the flip side of the coin, I HATE to give them the news they dreaded most, which is when the test result is negative.
This is the reality of IVF, you win some battles, and you lose some. We rejoice with the patients’ victories and we weep for their defeats.
For those battles that we lost, what is the next step forward?
We talked about the overall success rates of ONE IVF a few days ago and we know for sure that if you have a good number of embryos from the result of ONE IVF, the chance of you getting pregnant with the subsequent Frozen embryo transfer is extremely likely, especially if you are under the age of 35. In fact, there is some evidence to suggest that Frozen embryo transfers yields a higher pregnancy rate compared to fresh embryos transfers
(Rogue M at al. Fresh embryo transfer versus frozen embryo transfer in in-vitro fertilization cycles: a systematic review and meta-analysis. Fertil Steril. 2013 Jan;99(1):156-62)
However, if you have no embryos frozen, what is your option?
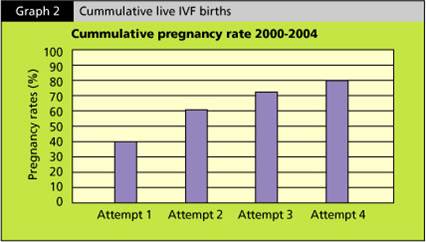
This chart below showed a cumulative live IVF births from a study conducted in Australia.
This study looked at all the women under the age of 42, who are going through IVF.
The study revealed that the pregnancy rate is around 40% in this group of women after they completed their first cycle of IVF. For those women who did not get pregnant the first round and went on having the second round of IVF, there were another 20% who got pregnant after the second round. Therefore, by the 4th IVF cycle, around 80% of women would have achieved a live birth.
This statistic clearly shows that if you persevere and keep moving on, chances of you getting pregnant by the end of the 4th IVF is around 80%.
Therefore, it is not unusual for Fertility doctors to encourage our patients to keep moving on because the statistics had clearly show us the evidence.
The Reality of IVF
Many couples choose their Fertility doctors because of their preference towards a characteristic of the doctor, however, many more choose to undergo their IVF treatment under a doctor or a centre because of the perceived success rates of the doctor or a centre. A published survey in the UK revealed that success rate of a centre or a doctor is the key determining factor for the decision of going through IVF in a particular Fertility Centre.
Therefore, all IVF doctors and centres strive very hard to increase the success rates of their patients. We emphasize on the patients’ lifestyle and age, in hope to get them to come at a younger age and in a better state of body fitness, so that we can obtain better eggs and sperms and hence make better embryos. We improve our laboratory environment and technology to mimic the uterus environment to yield a better fertilization and growth rate. We pat our own shoulders when we produce good quality embryos. And then we transfer the good looking embryos into the uterus and we wait……
10-12 days later, we either rejoice with the patient for a positive result, or we put on a very sad and sorry face to deliver the bad news
So what happened in between the time after we put those embryos back into the uterus until the time we test for pregnancy? The answer to this is that nobody knows.
As doctors we placed the embryos back, and nobody actually knows when and how the embryos get implanted, and what determines whether the embryos will get implanted or not.
This is the Holy Grill of the science and wonders of IVF
Many people had tried various things, complete bed rest, baby aspirin, steroids, hanging the legs up and etc etc etc.
Studies after studies failed to show any good recommendation on what we should do to improve the implantation rates. Some people believe that by performing a Pre-implantation Genetic diagnosis (PGD) can improve the implantation rates. There is some logic behind this: by selecting the normal chromosomal embryo to put back into the uterus, the chance of implantation increases. However, years had gone by with such a practice being implemented in some centers and there is only a marginal increment in pregnancy rates.
A recent study conducted at KL Fertility Centre (Monash IVF, KL) showed some interesting data.
We looked at all the women going through one IVF and divide them into 3 different groups by age.
Women who are under the age of 35 have 60% chance of getting pregnant during the fresh cycle when we put back the embryos into their uterus.
If they do not get pregnant during the first round and have good embryos which can be frozen and to be used in a later date, the chance of them getting pregnant by replacing 1-2 frozen embryos is around 60%.
By the time this group of women exhausted all their embryos which were produced by ONE IVF treatment, the likelihood of them having at least one baby is around 80%.
This translates that 4 out of 5 couples who are under the age of 35 will get pregnant with just ONE IVF attempt.
The success rate is about 60% in women between the age of 35-40 with the same trend observed.
Even for the group of women who are in the range of over 40 years of age, the success rate is close to 30%.
This certainly have a significant impact on the way we think….we now know that the chance of pregnancy is extremely good by just having ONE IVF without even having to subject the embryos to expensive and potentially hazardous pre-implantation genetic testing.
The key thing is to just keep moving on!!!!!

Age and IVF success rate
Many couples went through IVF in hope to have a child. Many view this treatment as the last resort to having a child. Therefore, it is not unusual for me to encounter couples who had exhausted ALL forms of treatment and landed in my clinic after many frustrating years. Some had come a bit too late….
Part of my job as an IVF specialist includes constantly being asked by patients on their chances of pregnancy by IVF.
This is definitely a relevant question. IVF is an expensive treatment and certainly after spending XYZ amount money on this treatment, you would like to know what is your chance of pregnancy.
In general, the chance of pregnancy depend on 3 most important factors: The woman’s age, the number of years of subfertility & whether there had been any pregnancies in the past.
Out of these three factors, the most important and relevant factor would be a woman’s age.
Studies had shown that after the age of 35, the chance of women getting pregnant naturally as well as through Fertility Treatment declined gradually. There is a further sharp declined after the age of 40.
I do not mean to press the panic button for all the women over the age of 35. However, I strongly feel that this is an important message which many Fertility Specialists like us had not been shouting loud enough to educate the general public.
Studies from Australia & US had shown that the success rate of an IVF is around 50% before the age of 35. The success rate drops thereafter and hit the range of 20-30% by the time the woman turns 40. The chance of pregnancy after the age of 44-45 is close to 0%.
The reason for a lower success rate after the age of 35 is a combination of the fact that age is associated with decrease number of follicles and quality of the eggs. For women, we are born with millions of eggs and the process of recruitment and activation of eggs started as we reached puberty. The number of eggs in our ovaries go down as we aged. By the time we each menopause, the eggs were completely depleted in our ovaries. Therefore, at the age of 35, we are expected to be producing less number of eggs. As we age, the quality of eggs also decrease and there is higher likelihood to produce eggs with abnormal chromosomes. Therefore, there is a higher risk of miscarriage and fetal anomalies.
A Ray of Sunshine
I received a call from Mrs Sunshine, one of my IVF patient, who informed me that she had delivered her baby a week ago via Caesarean section at 34 weeks due to severe intrauterine growth restriction. Although the baby was small in size, she was doing very well in the neonatal ICU, not requiring ventilation and was discharge after 3 days.
In December 2012, Mrs Sunshine came to see me for fertility assessment and treatment following 2 miscarriages (recurrent miscarriages). She is a slim and graceful lady with a beautiful smile. Along with her is her loving and understanding husband. They lived in Raub Pahang and every appointment required them to drive more more than an hour to get here.
Her previous 2 pregnancies ended at 5-8 weeks respectively with no evidence of fetal heart beat. Blood tests revealed no abnormalities. She decided to have an IUI under my care but unfortunately she did not get pregnant.
At that time, she started a blog called Wishing for a Sunshine: http://wishingforasunshine.blogspot.com/, which I was not aware of initially. In her blog, she carefully recorded her struggles with Fertility Treatment and all the ups & downs along the way. This is the first time, as a Fertility Specialist, I am able to have a clear insight of the perspective of a patient going through fertility treatment under my care. As a female fertility specialist, I always pride myself to think that I would understand how a woman feel especially in terms of the desire to have a child, but what strikes me is that sometimes, there are still certain personal struggles one faced whilst going through fertility treatment. As a doctor, I can now understand that comforting and reassuring words which I said, could give patients such confidence to move forward in the quest of having a child.
She went on with an IVF under my care and successfully got pregnant and have a few embryos frozen for later use. Although her pregnancy had not been easy, but it all turned out well eventually.
Months after her IVF, my other patients told me about her blog, which was very widely read by many. These patients unanimously told me how her story had greatly inspired them, motivated them to move on with Fertility Treatment.
Although Mrs Sunshine was wishing for a sunshine in her womb, but in fact, she herself had turned out to be a sunshine giving rays of hope for many threading the same journey.
My congratulations to Mrs Sunshine and a big thank you to her for blessing others in her special way!

Doctor, twins please!!!!
As a mother of a pair of twins, my patients are usually quite curious how I managed to conceive with a pair of twins. Most of them thought that I have been through an IVF myself.
However, the reality is that I did not need to do so. I came from a family blessed with many pairs of twins and there were even triplets (conceived naturally) in my family. Multiple pregnancies gene runs in my father’s family: My 5th & 6th uncles are twins, my 5th uncle went on having a pair of twin girls himself. My first uncle had triplets (conceived naturally) in addition to 6 other children he had (with just one wife, blessed). Nobody suspected that my aunt carried triplets until the second baby was born and the doctor found another baby in the womb. Of course we can’t criticize the doctors then because those days were the days before the advent of ultrasound scans and the use of ultrasound scans for pregnancy only came on 10-15 years later. My first aunt (my father’s only sister) have a pair of twin grand-daughters. If you search long and hard enough, and look thoroughly at my family tree, you will notice that my grandfather’s brothers and sisters are all blessed with twins in their family. If you take all these pairs of twins into consideration, you are talking about probably at least 10-15 pairs of twins in the lineage of my great-grandfather.
How did it happened? We have no idea. We used to think that one would inherit the multiple pregnancy genes through maternal lineage. However, my father’s family had challenged the popular belief. My father used to think that it was the water or the soil around the area where they lived. However, I don’t live near the area where the family came from and I don’t believe that my brief stays of 1-2 weeks yearly as a child at my ancestor home would have contributed to the incidence. My aunt who delivered the triplets did not live around the ancestor home either.
My interesting family history has pre-determined my destiny to be blessed with a pair of twins. And as I am blessed with a job of my dream to help to create babies in the field of Assisted Reproductive Medicine, my profile as a mother of twins has gradually become a fascination for my patients.
I have had many e mails from patients directed to me asking whether I could help them to conceive with a pair of twins.
I felt very privileged by their request but yet find this request daunting because even with all the Fertility Treatment which are available, there is still no guarantee that one could be pregnant with twins.
The incidence of twins is 1:80 pregnancies if you let nature run its course. If a woman takes Fertility pills such as Clomid (Clomiphene citrate) to enhance their fertility, the chance of conceiving a pair of twins is estimated to be around 5-10% if she fall pregnant. If she undergo ovulation stimulation coupled with an intra-uterine insemination (IUI), the chance of her pregnant with a pair of twins is around 10-15%. If she undergo In-vitro Fertilization (IVF), her chance of getting a pair of twins is around 20% if she have had 2 embryos replaced into her womb.
What patient needs to understand is that all Fertility Treatments increase the chance of having multiple pregnancies in different proportions but none will be able to guarantee the outcome.
Having twins is not without its complications. I always like to warn patients but I am not sure whether this goes down well with them. These complications are real but yet we as clinicians find it hard to present it to patients simply because it is not so palatable.
First and foremost, multiple pregnancy poses risk for the expecting mother. There are increased risk of complications such as:
(1) high blood pressure in pregnancy (I was a typical example of such complications, having had fulminant high blood pressure with presence of protein in my urine and required high dependency care and emergency Caesarean section at 33 weeks)
(2) High blood sugar in pregnancy (I escaped narrowly as my test result was near borderline)
(3) Low lying placenta or Placenta Praevia in pregnancy (That too was a concern until 28 weeks and my obstetrician, who happened to be my boss ordered me to stop work at 26 weeks)
(4) preterm delivery (Statistically, 60% of twins are born before 37 weeks. Some of the pre-term deliveries were attributed by the medical conditions in pregnancies which required early delivery)
(5) Anaemia in pregnancy
The risks for the babies include:
(1) Higher risk of miscarriage & stillbirth
(2) Higher risk of early neonatal loss. The risk of death for premature babies around the week of birth is five times higher for twins and nine times higher for triplets than single babies.
(3) Higher risk of prematurity and long stay in Neonatal Intensive Care Unit, half of all twins are born prematurely (before 37 weeks) and have a low birthweight of under 2.5kg (5.5lb); triplets have a 90% chance of being born prematurely and of having a low birthweight. My babies was taken to Neonatal ICu at birth and stayed for 16 days. It was the worst 2 weeks of of my life, having to go through the emotional roller costers for 2 weeks
(4) Higher risk of babies having Cerebral Palsy. Twins are four times and triplets 18 times more likely to have cerebral palsy than single babies.
As for the family, the burden would be:
(1) $$$ (Diapers , Milk Powder, and everything else that requires 2 sets at the same time)
(2) Childcare. Looking after a pair of twins who cried simultaneously, need feeding and changing simultaneously would drive a sane woman insane.
(3) Lack of ZZZZ. A chronic problem as you need to wake up more often in the middle of the night for feeding and changing the diapers
(4) Bigger car required. A MPV is required to fit in 2 car seats and a spacious boot to fit in a double baby prem
So, before you ask me to help you to conceive with a pair of twins, would you consider reading this article beforehand?